Zonulin – a marker for intestinal permeability
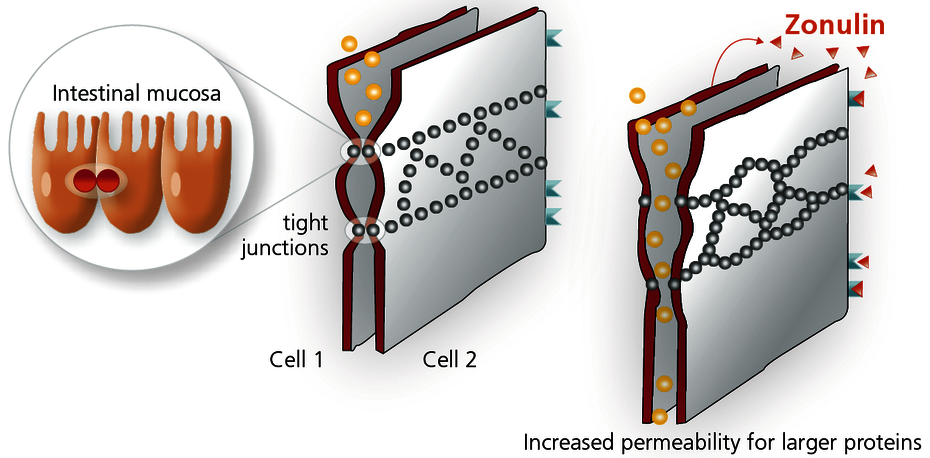
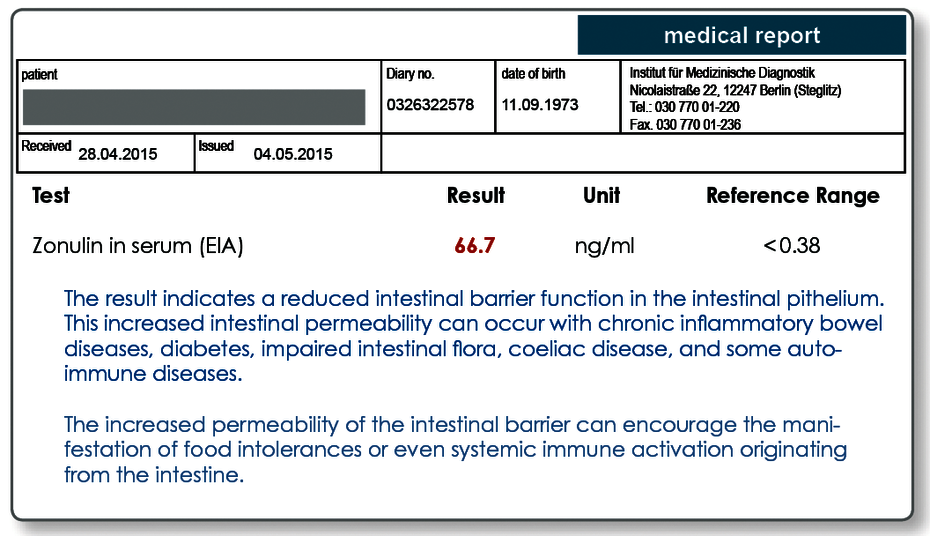
The epithelial cells in the intestinal mucosa are held together by narrow bands (called tight junctions). The tight junctions seal the spaces between the cells and ensure an intestinal barrier. They are regulated by the protein zonulin. After the intestinal mucosa is stimulated in different ways, zonulin is released and causes the opening of the interepithelial channels. Studies show that elevated levels of zonulin correlate with increased intestinal permeability. Analysing the zonulin level in the serum, with well-documented comparable evidence, allows the intestinal permeability to be analysed without the cost of a provocation (e.g. lactose/mannitol quotient).
Food intolerances are often secondarily the result of chronic inflammatory processes in the intestine. The resulting alteration in the intestine worsens the leaky gut condition, which means that increasing amounts of immunogenic (undigested) food components can break through. This causes existing sensitisations to then become clinically manifest (food allergy). At the same time, the additional confrontations with food allergens increase the likelihood of a sensitisation.
The intestinal epithelium is the location where enzymes such as diamine oxidase and lactase are synthesised, which is why morphological changes to the intestinal mucosa caused by inflammation also lead to reduced synthesis of these essential enzymes. Therefore, a secondary DAO deficiency (secondary histamine intolerance) or secondary lactase deficiency (secondary lactose intolerance) are often caused by chronic inflammatory bowel diseases.
The determination of zonulins is not only used to determine the status in the case of "leaky gut". It also allows monitoring of the course of treatment. For patients with coeliac disease, for example, the zonulin levels decrease in parallel with the inflammation parameters when a strict gluten-free diet is followed.
Material
Zonulin: 2 ml of serum
Literature
- Lammers KM et al. Gliadin induces an increase in intestinal permeability and zonulin release by binding to the chemokine receptor CXCR3. Gastroenterology. 2008;135:194-204.
- Sapone A et al. Zonulin upregulation is associated with increased gut permeability in subjects with type 1 diabetes and their relatives. Diabetes. 2006;55:1443-1449.
- Wang W et al. Human zonulin, a potential modulator of intestinal tight junctions. J Cell Sci. 2000;24:4435-4440.