Histamine Intolerance
| The clinical pattern of histamine intolerance (HIT) is defined as the exceeding of the individual histamine tolerance limit. Usually, this is caused by a lack of the histamine-degrading enzyme diamine oxidase (DAO). A decrease in activity of the second histamine-degrading enzyme histamine N-methyltransferase (HNMT) may lead to a worsening of symptoms. HIT may also manifest clinically if the organism is currently exposed to more histamine than it can degrade, despite normal DAO activity. Both a lack of DAO and an excessive exposure to histamine, can be detected with the help of laboratory diagnostic measures. In the case of proven lack of DAO, DNA testing is used to differentiate between primary and secondary causes. Furthermore, an activity-decreasing genetic HNMT variant can be detected. |
Histamine – the most important vasoactive mediator
Histamine is a biogenic amine, which is released by activated mast cells. Being a vasoactive mediator, it plays a dominating role in allergic diseases, such as Rhinitis allergica (hay fever), allergic bronchial asthma and urticaria (hives). Moreover, histamine is released in cases of pseudoallergies in conjunction with drugs or food additives, inter alia. In addition to endogenously released histamine, histamine is ingested with food.
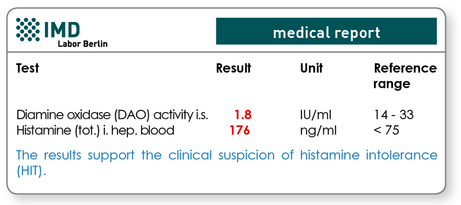
DAO activity and histamine concentration in blood are measurable
DAO is continuously released into the bloodstream, and hence the activity of DAO in blood serum is a suitable marker for HIT diagnoses. Measuring the intracellular HNMT, which occurs primarily in the liver, is, on the contrary, not possible. Here, the detection of an activity-decreasing genetic HNMT variant is available. HIT is nevertheless not only caused by the insufficient breakdown of histamine. It may also manifest clinically when there is a histamine surplus that is currently not broken down sufficiently, even under normal DOA activity. Allergic diseases, such as hay fever, sensitisation towards mould, and elevated levels of mast cell activity are sources of additional histamine that accumulates with ingested histamine. In order to diagnose this type of transgression of the individual histamine tolerance limit, DAO activity should be analysed together with the histamine total in blood.
Genetic testing differs between primary and secondary lack of DAO
In order to avoid unnecessary lifelong dieting, whether the existing lack of DAO is caused by a genetic primary, or a secondary condition, must be analysed. The result will then have an impact on the treatment. A primary lack of DAO is accompanied by decreased DAO activity, due to genetic variations (polymorphisms). Patients with proven decreased DAO activity in blood and corresponding clinical symptoms ought to receive genetic screening, in order to differentiate between a genetic or secondary, and therefore causally treatable and reversible, form of histamine intolerance.
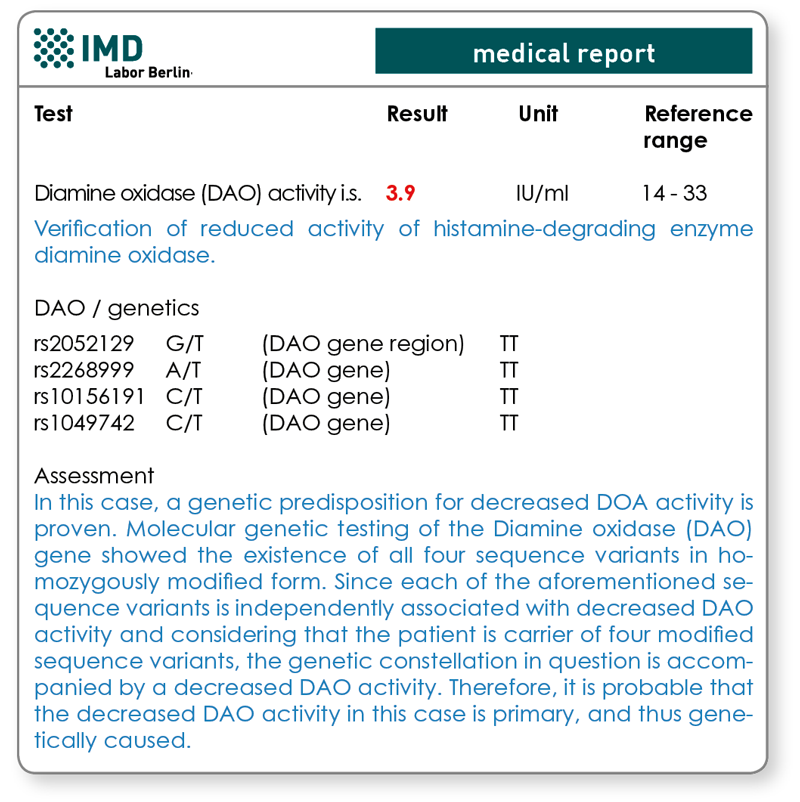
A common cause for a secondary lack of DAO are inflammatory or degenerative bowel diseases, because more than 90 % of DAO is produced in the intestinal epithelium. But also cases in which drugs, alcohol or toxins decrease the activity of DAO, are considered secondary forms. Drugs that have a proven record of decreasing DAO activity are mentioned below. Another possible cause for decreased DAO activity may be a copper deficiency, since copper constitutes DAO’s central atom and is hence vital for its performance.
Therapeutic consequences of reduced DAO activity
When decreased DAO activity or significantly elevated histamine levels are proven, foods rich in histamine have to be avoided. In the case of a secondary HIT, meaning a decreased DAO activity despite normal genetic makeup, the cause has to be identified (chronic inflammatory bowel disease? copper deficiency? prescription drug and alcohol history?), since secondary histamine intolerance is, unlike primary histamine intolerance, in most cases reversible. In patients with decreased DAO activity, copper levels should be monitored, in order to avoid an additional deterioration of the residual DAO activity due to copper deficiency. Simultaneously, zinc levels should be monitored, since zinc inhibits intestinal copper absorption. A merely symptomatic therapy through the prescription of H1 receptor antagonists should only be a temporary measure.
Known DAO-inhibiting drugs:
| Acetylcysteine | Cimetidine | Morphine |
| Alcuronium | Clavulanic acid | Pancuronium |
| Alprenolol | Cyclophosphamide | Pentamidine |
| Ambroxol | Dihydralazine | Pethidine |
| Amiloride | Dobutamine | Prilocaine |
| Aminophylline | Isoniazide | Propafenone |
| Amitriptyline | Metamizole | Thiopental |
| Cefotiam | Metoclopramide | Thiamine |
| Cefuroxime | Metronidazole | Verapamil |
| Chloroquine |
HNMT can have genetic causes or show decreased activity due to environmental exposures
While Symptoms of a lack of DAO are often periodical, symptoms of HNMT deficiency occur immediately after meals, for example. In the case of dysfunctional HNMT, especially the brain, bronchial mucosa and liver are affected. Patients with normal DAO levels, who experience only slow deterioration (days) of symptoms after dietary errors and in which after dieting properly symptoms abate only slowly, may suffer from HNMT deficiency. Testing the activity of this intracellular enzyme is not possible. Diagnostics are done via testing for a genetic variant (C314T) that decreases HNMT activity by 30-50 %. This genetic variant is associated with histamine-related diseases, such as asthma and atopic dermatitis. Additionally, drugs are known to be HNMT inhibitors. Amodiaquine, Metoprine, Tacrine and Diphenhydramine (H1-antihistamine!) block HNMT’s histamine binding sites. Carriers of C314T-polymorphisms should hence avoid HNMT blockers as well as histamine liberators.
Material
DAO activity: 2 ml serum
Histamine tot.: in blood: 10 ml heparin blood
For both tests, a sample receipt within 24 hrs has to be ensured. The sample should be stored and transported at room temperature. Within the Berlin city area, we offer a courier service (+49 (0)30 7701- 250). For collections beyond Berlin, please contact our complimentary courier service (+49 (0)30 77001-450).
DAO genetic testing and/or HNMT genetic testing:
2 ml EDTA blood
For genetic testing, the patient’s declaration of consent is mandatory. Transport to the laboratory is not time-sensitive and can be sent by mail.
Would you like to see a presentation on the matter?
In our video archive, you can find a free presentation on this topic. Access is free und possible without prior registration.
